Top Cosmetic, Family & General Dentist in Southern CA
OC Smile Family & Cosmetic Dental Office in Mission Viejo, CA & Fullerton, CA
If it has to do with your teeth and oral health, OC Smile can be your go-to dental facility. We do thorough examinations, take any required x-rays, and identify issues early on as cosmetic, family, and general dentists. In addition, we offer oral hygiene advice and complete dental cleanings.
We can assess problems and offer suggestions on various procedures when it comes to enhancing the appearance of your teeth. Our techniques include dental bonding, veneers, enamel shaping, and crowns to enhance the symmetry and alignment of our patients’ smiles. Gum shaping procedures can improve the appearance of a “gummy” smile, while other procedures can address receding gums. We also use whitening to make teeth that are yellow or discolored look better. We offer a wide range of in-house specialists for other speciality dental requirements, including orthodontics, implants, wisdom teeth extraction, pediatric dentistry, and much more, for smiles that need further reshaping.
When to Visit the Dentist
Many patients only visit the dentist when there is a problem. It is extremely unfortunate that they are skipping out on so many preventive services that might spare them future suffering and expense. Regular dental appointments are necessary to ensure that oral health issues, such as tooth decay and oral cancer, are identified and treated as soon as possible. Everyone should visit the dentist at least once a year, while some people may need to go more frequently to keep up with issues like plaque accumulation and gum disease than others.
A comprehensive oral exam to evaluate the condition of your teeth and gums, an oral cancer screening to identify any early warning signs, and a professional cleaning to get rid of lingering buildup and improve the appearance and feel of your teeth are all included in your routine dental visits. Don’t let dentistry’s many advantages pass you and your family by!
Mission Viejo, CA Dental Office – Top-Rated Cosmetic Dentists in Fullerton, CA
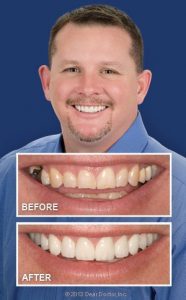
You’ll feel terrific when you have a confident smile. A beautiful and confident smile is a valuable social and professional benefit and asset. Many people, on the other hand, avoid showing their teeth in public or in photographs because they dislike what they see. If this describes you, a smile makeover is a great place to start when it comes to having the smile you’ve always desired.
A smile makeover involves more than just addressing dental issues as they emerge. It’s a thorough smile-rejuvenation strategy tailored to your specific facial characteristics and aesthetic preferences. Both in terms of how you look and how you feel, the results can be pretty astounding.These are the major steps involved:
Take a look around. The goal of the smile makeover is to give you the smile of your dreams. So take a close look at your grin and make a list of what you like and dislike about it. The following are some questions you can ask yourself:
- Are your teeth as white as you’d like them to be?
- Are any teeth chipped, cracked or worn?
- Does your smile have a gummy appearance?
- Do your teeth seem too large or small?
- Do you like the alignment and spacing of your teeth
- Are you self-conscious about crookedness or gaps?
Keep in mind that beauty is in the eye of the beholder… which is you! Some people desire their smile to be “perfect,” which they define as having perfectly straight, evenly white teeth. Others want a more natural look and are unconcerned about little gaps or shade differences. There are a lot of choices to make, but don’t worry – dentists are experts at guiding you through them.
Share your thoughts. The importance of communication in the smile makeover process cannot be overstated. It helps if you express what you want to modify in as much detail as possible during your initial makeover consultation. Bring images of smiles you like or of how you used to look when you were younger. Because dentists are trained to look at smiles in terms of facial balance, your makeover dentist will have some ideas to discuss with you. To put it another way, a dentist will consider not just how the components of a smile (teeth, lips, and gums) interact with one another, but also how they blend in with the rest of the face.
Make a plan. A comprehensive dental checkup is a crucial part of arranging a smile makeover. Cosmetic dentistry offers a wide range of lifelike dental restorations and treatments, but any issues in your mouth that could compromise a positive outcome must be addressed first. If your teeth are stained, for example, you must figure out why. Before whitening your teeth, you may have an underlying dental illness that needs to be treated; otherwise, the whitening may not persist. If you drink a lot of red wine or other staining beverages, porcelain veneers may be a better option than bleaching procedures.
Try it out. A smile makeover is an investment that will pay off in the long run. As a result, many of the operations are irreversible. So, if you’re thinking about making any modifications, it’s a good idea to try things out first before committing entirely. There are many ways to preview the results: computer imaging, 3-D models, and even placing temporary restorations on your teeth so you can see what the final results will look and feel like in your own mouth. This also enables the remodeling strategy to be fine-tuned.
A “trial smile” is a great way to eliminate unknowns in the makeover process. But when it’s all done, there’s still one thing you may not be prepared for: how great it feels to flash your new smile to the world!
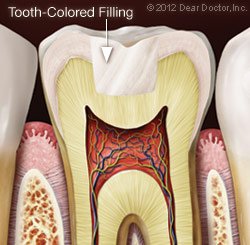
Congratulations if you have never had a cavity! You are not alone if you have had one. According to a 2000 report by the US Surgeon General, by the time we reach the age of 17, 78 percent of us have had at least one cavity. Fortunately, there is a tried-and-true cavity treatment: dental fillings.
Fillings accomplish precisely what their name implies: they seal a small cavity in your tooth caused by decay. This prevents the decay (a bacterial infection) from progressing deeper into your tooth and, if left untreated, to the root canal’s sensitive inner pulp (nerve) tissue. You’ll need root canal therapy if this happens.
A clinical examination of the tooth with x-rays is the first step in determining the degree of the decay. The decaying portion of the tooth is then removed, commonly using a portable device like a dental drill. Naturally, your teeth will be sedated beforehand, so you will not be in any pain. If you’re apprehensive about getting numbing injections, anti-anxiety medicine or nitrous oxide may help you feel more at ease. After the decay is removed, the remaining tooth structure is roughened or “etched” using a mildly acidic solution, followed by the application of translucent cement to fuse the tooth and the filling material together.
Types of Fillings
There are two broad categories of dental fillings: metal fillings and tooth-colored, composite fillings. Each one offers particular advantages and disadvantages in certain situations.
Metal Fillings
Amalgam — Dental amalgam, the classic “silver” filling that has been in use for over a century, is actually an alloy made composed of mercury, silver, tin, and copper. The mercury in the amalgam combines with the other metals to make it stable and safe. These fillings are robust and affordable, but they are also conspicuous. In addition, they necessitate greater tooth preparation (drilling) than other varieties.
Cast Gold — Cast gold is one of the most expensive restorative dental materials because it blends gold with other metals to create a filling that is extremely robust and long-lasting. It’s also very obvious, which might be a benefit or a disadvantage.
Tooth-Colored Fillings
Composite — A popular choice for those who don’t want their fillings to show, composite is a material made up of plastic and glass that adheres to the remainder of the tooth. Composite fillings are more expensive than amalgam fillings, but they last almost as long. When compared to amalgam, installing composite requires less drilling of the tooth.
Porcelain — These high-tech dental ceramics are durable, realistic, and stain-resistant, unlike composites. Because they may necessitate the use of a dental laboratory or specialized computer-generated technologies, they can be more expensive than composites. While they are the most attractive filler, they can also be brittle due to their relatively high glass content.
Glass Ionomer — These low-cost, transparent fillings are made of acrylic and glass powders and have the advantage of blending in nicely with natural tooth color while also releasing small amounts of fluoride to help prevent decay. They don’t usually last as long as other types of restorative materials.
What to Expect After Getting a Filling
The numbness caused by your local anesthesia should wear off within a couple of hours. Drinking hot or cold liquids and chewing on the side of your mouth with the new filling should be avoided until then. In the first few weeks following having a tooth filled, some sensitivity to hot and cold is usual. If discomfort persists after that, or if you experience any genuine pain when biting, it may indicate that your filling needs to be adjusted. Continue to brush and floss as usual every day, and schedule routine dental examinations and cleanings at least twice a year. Remember that tooth decay is a disease that can be avoided with proper oral hygiene and professional care; your most recent cavity can be your last!
Dental crowns are a fantastic example of how dentistry is both an art and a science. A dental crown, sometimes known as a “cap,” is a cap that fits over a broken, decaying, or unsightly tooth. As part of dental bridgework, it can potentially completely replace a tooth.
A crown entirely covers a tooth above the gum line. In contrast, a dental veneer merely covers the front surface of a tooth and is supported by natural tooth structure. If a tooth has lost a significant amount of structure above the gum line, a crown would be the best option for restoration.
Crowns protect and reinforce injured teeth, allowing them to resume normal function. Crowns are essentially indistinguishable from natural teeth when made with today’s high-tech porcelains (dental ceramics). They can even be designed to improve the appearance of a tooth.
Other materials can be used to construct dental crowns than porcelain, depending on the properties that are most significant. Cast gold is unrivaled in terms of durability. However, especially near the front of the mouth, this is not usually the most attractive option. Other options include porcelain-fused-to-metal (PFM) crowns, which contain a metal interior for strength and a porcelain exterior for a more natural look, and all-porcelain crowns with zirconia, the strongest ceramic. We’d be pleased to go over the advantages and disadvantages of these various solutions with you.
Crowning or Capping a Tooth
It normally takes two to three appointments to crown or cap a tooth. Your tooth gets prepped for its new crown during the first visit. It’s first shaped to fit within the new cover. Drilling will be required to give the tooth a uniform shape. Before the procedure, the tooth and the surrounding area will be numbed. To support the crown, the tooth may need to be built up with filler material rather than filed down if there is very little dental structure left to begin with.
After the tooth is prepared, digital or putty-like imprint materials are used to take impressions of your teeth, which are then sent to the dental laboratory. The impressions will be used to create models of your teeth so that a crown may be made. The models will be used as a guide for the highly trained lab technicians who will guarantee that your new crown is made to complement your smile while also functioning properly within your bite.
A temporary crown will be placed on your tooth before you leave the office to safeguard it until the permanent crown is ready. Your permanent crown will be cemented to your tooth at the second visit, either using a resin that solidifies when exposed to a particular light source or with a form of permanent cement.
Creating a Bridge
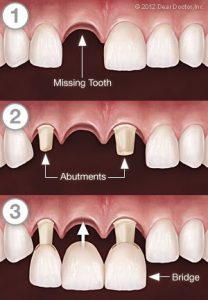
Crowns can also be utilized to replace a missing tooth in a lifelike manner. Bridgework, which spans the gap left by the lost tooth and requires at least three crowns, is used to accomplish this. Two of those crowns will be placed over healthy teeth on either side of the missing tooth, known as abutment teeth. The two capped abutment teeth serve as supports for a pontic, which is a third crown that is inserted between them. More crowns will be required to bridge the space between the abutment teeth if more than one tooth is lost.
The number of abutment teeth required to replace missing teeth is determined by the number of missing teeth, the size and length of abutment tooth roots, the amount of bone support provided by each abutment tooth, and the location of the missing tooth in the mouth. If you have three missing teeth, for example, four abutment teeth may be required, resulting in a seven-tooth bridge. Understanding how to replace teeth, as well as the biology of the supporting gum and bone tissue, is required for bridge engineering and construction.
Caring for Your Crowns & Bridgework
Crowns and bridges demand the same level of attention as natural teeth. Brush and floss between all of your teeth, restored and natural, every day to prevent dental plaque buildup. Maintaining your normal dental cleaning plan becomes even more vital when you have crowns. Use your teeth as a tool as little as possible (to open packages, for example). Wearing a nightguard to safeguard your teeth and your investment is an excellent idea if you grind your teeth.
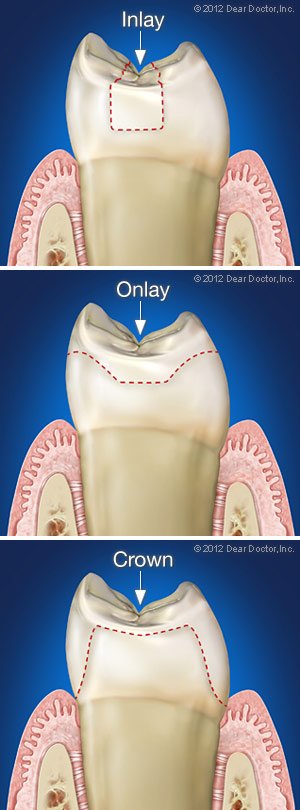
There are situations when a tooth suffers damage (such as decay) that is too severe to be addressed with a simple filling but not severe enough to necessitate a full-coverage crown. In these circumstances, an inlay or onlay may be the best option for repairing the tooth.
Both inlays and onlays are referred to as “indirect” fillings because they are created outside of the mouth (usually in a dental laboratory) and then glued to the tooth by the dentist. A “direct” filling, on the other hand, is placed directly to the cavity by the dentist in one office visit.
When an indirect filling fits into the little points or “cusps” of a rear (premolar or molar) tooth, it is called a “inlay.” If it covers one or more of these cusps, it’s called a “onlay.” The method for inserting an inlay or onlay is the identical in either case.
How Inlays & Onlays Work
When you get an inlay or onlay, it’s quite similar to getting a crown, with one crucial difference: less of your natural tooth structure will be removed through drilling when you get an inlay or onlay. When you acquire a crown, the tooth must be reshaped significantly in order to fit inside its new covering. Inlays and onlays may be advised instead of crowns when a tooth may be restored with this more conservative type of treatment, as dentistry’s goal is to retain as much of your natural tooth structure as possible.
The first step in receiving an inlay or onlay is to use a local anesthetic to numb the tooth and surrounding area before removing the decay. This is done to keep the decay, which is actually a form of infection, from spreading farther into the tooth.
Following the preparation of the tooth, an impression is taken (either digitally or using a putty-like material) and submitted to the dental laboratory. The impression is then used to create a model of your teeth for the inlay/onlay to be made. Gold, a tooth-colored porcelain, or resin might be used for the final restoration.
A temporary filling will be placed on your tooth before you leave the office to safeguard it until the permanent restoration is ready. The permanent inlay/onlay will be connected to your tooth at your second appointment, either using a resin that solidifies when exposed to a particular light source or with a sort of permanent cement.Inlays and onlays are durable, long-lasting restorations that require no more attention than any other tooth. All you need is diligent daily brushing and flossing, as well as frequent expert cleanings at the dentist, to ensure that your restoration lasts for years.
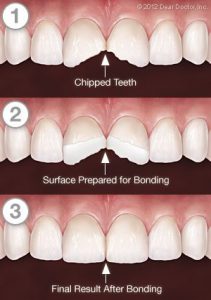
We are proud of how dentistry can restore broken or decayed teeth to their original beauty and function. Dental bonding is one of the simplest and least expensive ways to accomplish this.
Bonding is a cosmetic dentistry procedure that employs tooth-colored materials to repair missing tooth structure or conceal cosmetically undesirable tiny flaws in a tooth, such as chipping, discolouration, and minor spacing irregularities. Composite resins are bonding materials that comprise a blend of plastic and glass, which adds strength and transparency. The composite actually attaches to the rest of the tooth and becomes one with it.
For fully lifelike effects, composite resins are available in a number of tooth colors. It may be impossible to differentiate the bonded tooth from its neighbors when bonding is done with a skillful touch and an artistic eye. Though bonding does not last as long as a dental veneer, it does not necessitate the use of a dental laboratory and can sometimes be completed without the need for drilling. It’s an especially good option for teenagers, who must typically wait until their teeth have fully matured before deciding on a more permanent dental treatment.
The Dental Bonding Process
Because it does not involve dental laboratory work, tooth bonding can usually be accomplished in a single visit to the dental office. Expect the whole procedure to take 30 minutes to an hour. First, the surface of the tooth to be bonded will be cleaned so it is plaque-free. After that, the surface will need to be “etched” using an acidic gel to open up microscopic pores. After rinsing off the etching gel, a thin coating of liquid composite resin in a color that matches the etching gel is painted on, filling the microscopic pores and forming a strong micromechanical bond. This bonding compound is hardened using a specific curing light. After the first coat has dried, a second layer is applied and dried. Layers can be added until the restoration reaches the required thickness. A dental drill is then used to mould the bonding material into the desired shape. A final polish will be applied after the tooth not only looks wonderful but also fits correctly in your bite.
Caring for Bonded Teeth
Bonded teeth should be brushed and flossed daily, and professionally cleaned at the dental office twice per year, just the same as the rest of your teeth. The most important thing to keep in mind about caring for your bonded tooth is that composite resin can absorb stain, just as natural teeth can. As a result, you should avoid smoking, red wine, coffee, and tea to the greatest extent feasible. Additionally, composite can darken but not lighten. It, if you’re thinking about having your teeth whitened, do so before they’re bonded so that a composite shade that matches the lighter color of your whitened teeth can be chosen. If you whiten your teeth after bonding, the bonded tooth may not blend in with the rest of your teeth. Finally, avoid biting your nails, holding writing implements in your mouth, or otherwise using your teeth in ways that could cause the bonding material to chip. A bonded tooth should last 3 to 10 years if properly cared for.
 Full or partial tooth loss, if left untreated, doesn’t just affect a person’s self-image —
Full or partial tooth loss, if left untreated, doesn’t just affect a person’s self-image —
It can also raise the risk of having dietary issues as well as other systemic health problems. Fortunately, complete or partial dentures are a tried-and-true approach of managing this disease.
Fixed bridgework and dental implants are two further options for restoring missing teeth besides dentures. Each strategy has its own set of advantages and disadvantages that should be carefully considered. Dentures come in a variety of styles to address specific difficulties, ranging from partial dentures to implant-supported overdentures. The best solution for you will be determined by your unique circumstances.
How Do Removable Dentures Work?
It can also increase the chance of dietary disorders and other systemic health issues. Complete or partial dentures, fortunately, are a tried-and-true method of treating this illness.
Aside from dentures, fixed bridgework and dental implants are two further possibilities for replacing missing teeth. Each technique comes with its own set of benefits and drawbacks that must be carefully weighed. Dentures range from partial dentures to implant-supported overdentures, and are available in a number of styles to address specific problems. Your specific circumstances will determine the best answer for you.
As the dentures become “balanced” in the space formerly occupied by the teeth, wearing dentures may take some getting used to in terms of talking and eating. However, the mouth’s muscles, nerves, and ligaments learn to work in new ways during time, allowing these activities to perform regularly. Dentures also support the bones of the face as well as the soft tissues of the lips and cheeks, resulting in a more youthful appearance.
Types of Dentures in Fullerton & Mission Viejo
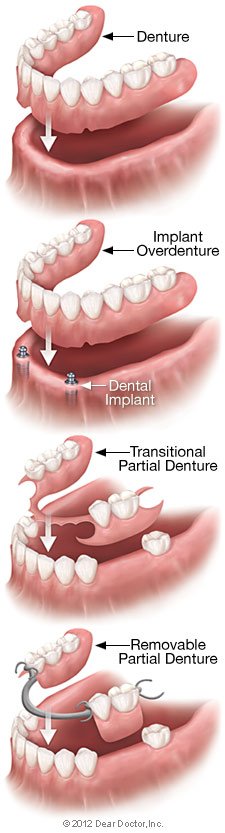
Immediate Dentures: These are usually only temporary aids in assisting you in making the transition to successful denture use. Dentures implanted immediately after tooth extraction will not fit as well as permanent dentures manufactured after recovery is complete due to the muscular re-adjustment necessary, as well as natural gum shrinkage. They do, however, immediately replace your teeth and allow you time to acclimate.
Conventional Full Dentures: Permanent dentures that adapt to your mouth with near-perfect accuracy can be created after a period of time. These are meticulously constructed to look as close to your actual teeth as possible, and they can last a long period in your mouth.
Implant-Supported Overdentures: It is feasible to securely anchor a lower or top denture using two or more dental implants to strengthen its stability. Due to decreased bone density, the upper jaw requires more implants (usually three or more) than the lower jaw. This option appeals to many individuals since it strikes a good balance between comfort, functionality, and price.
Types of Partial Dentures
Transitional Partial Dentures: These low-cost removable plastic dentures can be used as a temporary tooth replacement and space maintainer while your mouth heals from a tooth extraction, for example. Dental implants can be inserted after the healing process is complete.
Removable Partial Dentures (RPDs): These well-constructed metal-based detachable partial dentures, which are usually made of cast vitallium, are much lighter and less noticeable than those made of plastic. They are pricier than plastic dentures, but they will fit better. They are, however, a fraction of the cost of implants or fixed bridgework.
How Dentures Are Made and Fitted
Denture fabrication is a combination of science and art. The alveolar ridges on the top and bottom of your mouth are first accurately imprinted (molded). This mold is used to create the base of the denture in a dental laboratory. The dentist and lab technician collaborate to choose from a variety of sizes and forms of prosthetic teeth to re-create a natural-looking grin. When everyone is happy with the outcome, the temporary dentures are transformed into permanent dentures.
It’s critical to balance your bite in order to speak and eat normally. This indicates that the upper and lower dentures are appropriately aligned and stabilized. Dentures are meticulously examined for form and function to verify that they are functional and fitting appropriately.
What to Expect After You Get Dentures
It’s common to have some tissue shrinking and bone loss if you’ve just lost your teeth and received an instant denture. As a result, your immediate dentures may no longer fit properly after a few months. At this moment, you have two options: Your immediate (temporary) dentures can be re-lined. This means that under the denture’s foundation, material is introduced to better adhere to the altered shapes of your alveolar ridge. Moving to a set of traditional complete dentures, which will last longer and fit better, is a better option. Dentures provide a practical, cosmetic, and cost-effective solution to tooth loss when properly cared for.
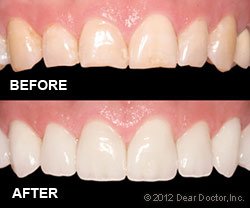 What makes a smile beautiful? That’s a complex question,
What makes a smile beautiful? That’s a complex question,
However, some characteristics of a beautiful smile are instantly recognizable: good tooth color, shape, and alignment are only a few of the most significant. If you’re looking for a way to improve any of these aspects of your smile, porcelain veneers might be the answer.
A veneer is a thin layer of material that is applied on the top of another surface. In dentistry, a veneer is a wafer-thin layer of super-strong porcelain that effectively substitutes natural tooth enamel. When attached to your teeth, veneers can create a natural-looking, gorgeous new surface. Like natural tooth enamel, dental porcelain is transparent and robust. It does not, however, discolor like tooth enamel.
Dental porcelain technology has advanced dramatically in recent years. Veneers can now be created so thin that they can be attached straight to the surface of your natural teeth. In other circumstances, a very thin layer of tooth enamel — as thin as the veneer itself — must be removed in order to suit the new porcelain surface and make it appear as natural as possible. In any case, the end product will make you happy.
Versatility of Porcelain Veneers
Veneers can be used to improve any of the following characteristics of your teeth:
- Color — Teeth can become discolored as a result of the foods and drinks we consume, as well as smoking and normal aging. Veneers come in a variety of colors, ranging from natural to dazzling Hollywood white.
- Size & Shape — Teeth might become worn down as a result of grinding behaviors, or they may be the wrong shape or size to begin with. Some people believe that rounder teeth are more feminine while squarer teeth are more manly. Veneers can be sculpted and fitted to fit your face in the most attractive way possible.
- Alignment & Spacing — Veneers can be used to repair small gaps between teeth or to make minor alignment changes while also improving the color and contour of the teeth.
Limitations of Porcelain Veneers
Veneers are not suited in various cases. If you have severely misaligned teeth or a huge gap between them, orthodontics may be a better option than veneers. If you’ve lost a lot of tooth structure due to disease or trauma (or a particularly bad grinding habit), ceramic crowns that cover the entire tooth may be a better option.
Creating a New Smile with Porcelain Veneers
The first step in transforming your smile with porcelain veneers is to express exactly what you don’t like about your current grin. Bringing in images of grins you enjoy as a starting point for conversation is a terrific idea. You may view how veneers would look on your teeth in a variety of ways. A model of your teeth can be made over which wax “veneers” can be applied; acrylic (plastic) or tooth-colored filling material can also be applied directly to your teeth to simulate the effect veneers might have.
If necessary, your teeth will be prepped by removing a little bit of enamel after the plan has been agreed upon. Molds of your teeth will be obtained and used by a competent dental laboratory to construct your veneers, and you’ll be given a temporary set to wear while your permanent veneers are being created. The veneers will be cemented onto your teeth after they arrive from the lab.
Caring for Your Dental Veneers
Just like the teeth nature gave you, gentle brushing and flossing are required for teeth restored with veneers. This will remove tooth plaque and maintain the health of the gum tissue around the veneers. Regular dental exams will remain as crucial as ever for your oral and overall health. Also, as durable as veneers are, they may not be able to withstand forces such as using your teeth as tools (to open packages, for example) or biting into really hard things like candy apples – which isn’t healthy for your natural teeth! If you grind or clench your teeth at night, a custom-made nightguard may be recommended to safeguard your veneers – and your investment.
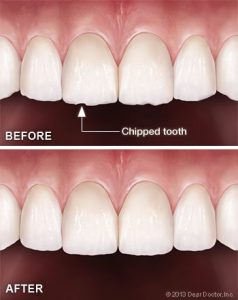 Sometimes little defects in teeth can attract more than their fair share of attention.
Sometimes little defects in teeth can attract more than their fair share of attention.
The small chip in a front tooth, the modest mismatch in tooth size among adjacent teeth, and the extra-pointy canine all appear to catch the eye. If you find yourself staring at these minor but irritating flaws in your own smile, help is available – often in the form of teeth contouring, a minimally invasive and reasonably affordable surgery (reshaping).
Tooth contouring entails using a drill to remove a little piece of tooth enamel in order to sculpt a more appealing shape and make the tooth blend in better with its neighbors. After that, the tooth is polished to make it as smooth as possible. The treatment is most commonly done on your most conspicuous teeth, the upper front incisors and canines.
Small chips, uneven tooth length, tiny overlaps, and tooth edges that are excessively flattened or pointed are all cosmetic issues that can be addressed by dental contouring. It can even be used to treat minor bite issues caused by teeth that come into contact unevenly. Reshaping your teeth, on the other hand, should be avoided if it could result in bite imbalances. One of numerous additional highly effective cosmetic dental operations might be suggested in that circumstance. Simply by rounding or squaring the corners, tooth contouring can be used to give teeth a more feminine or masculine shape.
What to Expect With Tooth Contouring
The initial step in the contouring operation is to inspect your teeth and determine how the reshaping will achieve your smile enhancement aim or fix any bite issues you may have. This ensures that the teeth being reshaped are not just attractive but also healthy. To protect you from gum disease, you may need to have your root surfaces reshaped. An x-ray may be required in this scenario to separate and protect the sensitive inner tissue (the pulp). However, tooth contouring usually only entails the removal of a little amount of enamel (the tooth’s hard outer layer). You won’t require a local anesthetic because enamel isn’t alive and doesn’t contain nerves.
As your teeth is gently molded and then polished smooth, you may most likely feel some vibration. One tooth can be reshaped in less than half an hour, and the results are visible as soon as you glance in the mirror! After the surgery, reshaped teeth may be slightly sensitive to hot or cold, although this should only last a day or two.
For a substantially younger-looking smile, tooth contouring can be combined with whitening. It’s also frequently combined with cosmetic bonding or dental veneers, which can also be utilized to remodel teeth with significant flaws.
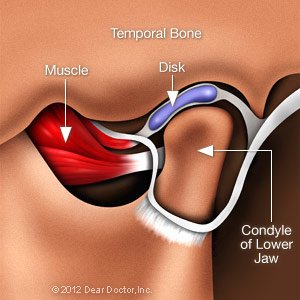 TMD – an abbreviation for Temporomandibular disorders — is defined as persistent pain in the area near your ear, jaw, or muscles on the side of your face, which may be accompanied by a clicking or popping sound or restricted jaw mobility. TMJ is the abbreviation for the temporomandibular joint — or jaw joint — itself, which is sometimes wrongly used to refer to these issues. So, while you do have a TMJ (in fact, two of them), you may or may not have TMD.
TMD – an abbreviation for Temporomandibular disorders — is defined as persistent pain in the area near your ear, jaw, or muscles on the side of your face, which may be accompanied by a clicking or popping sound or restricted jaw mobility. TMJ is the abbreviation for the temporomandibular joint — or jaw joint — itself, which is sometimes wrongly used to refer to these issues. So, while you do have a TMJ (in fact, two of them), you may or may not have TMD.
TMD, then, refers to a collection of conditions marked by discomfort and dysfunction of the TMJ and/or adjacent muscles. It’s not always easy to pinpoint exactly what’s causing these symptoms, but the good news is that most TMD cases recover on their own with the use of simple home treatments. In fact, before pursuing anything permanent, such as bridgework or surgery, it’s critical to exhaust all reversible options.
The TMJs, which connect your lower jaw, the mandible, to the temporal bone of your skull on either side, are actually incredibly complicated joints that allow three-dimensional movement. With a cushioning disk in between, the lower jaw and temporal bone fit together like a ball and socket. The lower jaw is moved by large muscles in the cheeks and temples. TMD can be caused by any of these components: the disk, the muscles, or the joint itself. A comprehensive examination will assist determine the issue location if you are in pain or having difficulty opening or shutting your jaw, and then a suitable solution can be prescribed.
Causes of TMD & TMJ
The TMJ, like any other joint, can suffer from orthopedic issues such as inflammation, aching muscles, strained tendons and ligaments, and disk issues. Genes, gender (women appear to be more susceptible), and age all play a role in TMD. Stress, both physical and psychological, might play a role. Jaw pain can sometimes be linked to a more widespread, pain-inducing medical disease like fibromyalgia. (“fibro” – connective tissues; “myo” – muscle; “algia” – pain).
Signs and Symptoms of TMD
Clicking Sounds — When opening or closing the mouth, some persons with TMD hear a clicking, cracking, or grating sound emanating from the TMJ. This is usually caused by the disk migrating within the joint. It’s possible that someone standing next to you can hear it. Studies suggest that one-third of the population has clicking jaw joints. TMD is indicated if the clicking is accompanied by pain or reduced jaw function, such as the jaw becoming “stuck” in an open or closed posture.
Muscle Pain — The two large pairs of jaw-closing muscles, the masseter and temporalis muscles, can be felt in the cheeks (masseter muscles) and temples (temporalis muscles). When you wake up in the morning, you may experience soreness and stiffness as a result of nighttime activities such as clenching and/or grinding your teeth. If you have this type of nocturnal behavior, a custom-made nightguard can help you reduce the force applied to your teeth, allowing your muscles to rest and relieve strain on your jaw joints. Other self-care options are addressed further down.
Joint Pain — The pain that comes from one or both jaw joints is properly referred to as TMJ arthritis (“arth” – joint; “itis” – inflammation). Some persons have arthritic-looking TMJs but no complaints of pain or dysfunction on radiographs, whereas others have considerable symptoms of pain and dysfunction yet their joints appear normal on radiographs. Although there is no cure for arthritis in any part of the body, medicines can help alleviate arthritic symptoms.
Relieving TMJ Pain
Following your examination, a treatment plan for your disease and pain management can be devised. A temporary switch to a softer diet can sometimes relieve muscular and joint stress. Soreness and inflammation can be relieved with ice and/or moist heat. Gentle stretching exercises might also aid muscles that are spasming. Muscle relaxants and nonsteroidal anti-inflammatory medicines can also help.
Other Treatment Options
Severe TMD instances may necessitate more complex treatments, such as orthodontics, dental restorations such as bridgework, or minor joint surgeries such as cortisone injections or joint lavage (flushing). Major surgery is rarely required in the treatment of TMD. Again, it’s critical to attempt a variety of conservative, reversible treatments and give them enough time to work since they almost always work. An examination at the dentist’s office is the first step.
 You already know how important a good night’s sleep is for good health. It makes you feel refreshed and ready to face the challenges of life. Despite this, many people do not get enough sleep. This is sometimes linked to sleep-related breathing disorders (SRBD) — either their own or those of their sleeping partners.
You already know how important a good night’s sleep is for good health. It makes you feel refreshed and ready to face the challenges of life. Despite this, many people do not get enough sleep. This is sometimes linked to sleep-related breathing disorders (SRBD) — either their own or those of their sleeping partners.
Recurrent episodes of decreased or interrupted respiratory airflow characterize SRBD. This is caused by soft tissues towards the back of the throat collapsing and partially closing up the windpipe while sleeping. These tissues, such as the tongue, can vibrate as air passes by, resulting in snoring. Sleeping on one’s back can exacerbate snoring because it promotes the lower jaw to slip back, pushing the tongue in front of the airway.
Snoring & Sleep Apnea Treatments in Fullerton & Mission Viejo
Loud snoring frequently wakes up the person in the bed who isn’t snoring, depriving him or her of essential sleep. On the other side, the snorer may appear to be sleeping comfortably, although this is not always the case. Chronic loud snoring is a common symptom of Obstructive Sleep Apnea (OSA; “a” – without; “pnea” – breath), which happens when the upper airway is closed to the extent that there is no airflow for 10 seconds or longer. Reduced airflow through the lungs lowers blood-oxygen levels, which can be harmful.
A person with sleep apnea may wake up 50 or more times each hour — nearly once every minute! — with no recollection of anything. Micro-arousals are brief awakenings that only last long enough to restore muscular tone to the airway, allowing the person to breathe. Unfortunately, all of those micro-arousals keep you from getting a good night’s sleep.
What to Look Out For
Obstructive Sleep Apnea (OSA) is a dangerous condition that can cause cardiac problems and other health problems. If you snore and have one or more of the following symptoms, you may have OSA.
- Excessive daytime sleepiness
- Irritability
- Poor memory/confusion
- Accident proneness
- Night sweats
- Morning headaches
- High blood pressure
- Obesity
How Dentistry Can Help
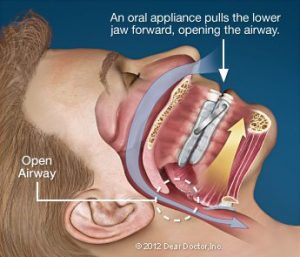
You’re probably thinking to yourself, “What does my dentist have to do with any of this?” Here’s how it works: Snoring or sleep apnea can occasionally be addressed using an oral appliance, which is meant to hold the lower jaw forward during sleep and is available at the dentist’s office. The tongue is moved away from the back of the throat by this displacement of the jaw, lowering the risk of obstruction. This treatment is backed by a lot of scientific evidence, so it’s a smart option to try before going on to more complicated breathing equipment or throat surgery to remove excess tissue.
Oral Appliance Therapy, which is used to treat SRBD, can only be made, fitted, adjusted, monitored, and treated by a dentist. So, if you or a loved one are suffering any of the above signs and symptoms, it’s a good idea to schedule an appointment with a dentist.
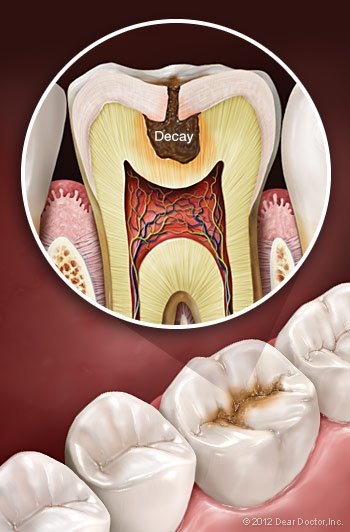 After the common cold, tooth decay is generally referred to as the second most common human ailment. It can lead to pain, tooth loss, and even severe ailments if not treated properly (as it has for much of history). Even today, it is estimated that one-quarter of American children aged two to five, and half of those aged 12 to 15, are affected. It does not, however, have to! You may take efforts to protect your teeth — and those of your loved ones — against dental decay.
After the common cold, tooth decay is generally referred to as the second most common human ailment. It can lead to pain, tooth loss, and even severe ailments if not treated properly (as it has for much of history). Even today, it is estimated that one-quarter of American children aged two to five, and half of those aged 12 to 15, are affected. It does not, however, have to! You may take efforts to protect your teeth — and those of your loved ones — against dental decay.
There’s one thing you should know right away: no single “magic bullet” can prevent tooth decay in every circumstance. Instead, battling decay should be considered as a form of preventive maintenance, similar to caring for your car – except that, unlike a car, your natural teeth can last a lifetime if properly cared for. The most important components of this process are good oral hygiene at home and regular cleanings and checkups at the dentist’s office.
You’re probably already aware with the special instruments dentists use to remove plaque (a bacterial biofilm) and tartar (a hardened deposit, also known as calculus) from your teeth if you’ve gone to the dentist for routine checkups. To thoroughly clean your teeth, hand-held devices, ultrasonic scalers, or both may be employed. Following that, your teeth are thoroughly examined for decay and, if necessary, cavities are treated.
There’s still more that can be done to keep teeth from decaying. Could your eating habits be a factor? Is your scrubbing method up to par? Is it possible that you could benefit from further preventive treatments? With a better grasp of what causes tooth decay and how to treat it, we can now concentrate on what decay prevention strategies will work best for you. In reality, it’s now able to examine each person’s decay risk factors and focus on what’s most beneficial for them.
How Does Tooth Decay Start?
It’s important to conceive of the mouth as a dynamically balanced ecosystem where live species, including both beneficial and dangerous bacteria, are continually interacting. Some pathogenic bacteria release acids that cause teeth to lose minerals and begin to break down when the conditions are appropriate, such as when certain carbohydrates are present. Demineralization of your teeth can be influenced by a diet high in acidic foods. However, in more favorable circumstances, the body’s own healing processes — including your healthy saliva — reverse the damage that these bacteria cause.
One of the most important goals in decay prevention is to shift the scales in favor of good activities. Brushing and flossing on a regular basis, obtaining enough fluoride, and eating a diet low in acidic foods are all beneficial. Even with these precautions, some people are more susceptible to tooth decay than others, and they may require further assistance and supervision.
Additional Steps to Prevent Tooth Decay
If you’re one of these people, learning good brushing techniques and practicing other steps at home, such as using specific toothpastes or mouthrinses, may be beneficial. In-office treatments, such as topical fluoride applications, are offered when needed. This therapy can help prevent tooth decay if you don’t get enough fluoride from your drinking water or other sources. In rare circumstances, antibacterial treatments and nutritional counseling may be effective.
Finally, if your child’s teeth are susceptible to decay, a dental sealant may be applied. On the top (chewing) surfaces of the back teeth, a nearly undetectable covering of plastic resin is applied. It’s a painless process that fills in the tooth’s natural pits and folds, making them far more resistant to bacterial attack.
So, rather than accepting that tooth decay is unavoidable, learn what you can do to assist prevent it from impacting you or your loved ones.
Meet Your Award-Winning Dentists in Mission Viejo & Fullerton, CA






Our Dental Services
General Dentistry
Dental Implants
Emergency Care
Pediatric Dentistry
Oral Surgery
Orthodontics
The Proof is in our Patients











